 You can read the revised article in the book:
You can read the revised article in the book: Introduction to Medical Equipment Repair The book also contains a chapter on preventive maintenance, with recommendations on how to perform the various tests. Click here for more information. |
Autoclaves |
by Frank Weithöner |
All surgical instruments that are in touch with open wounds or enter the body of a patient must be sterile. Therefore, all surgical instruments and materials have to be sterilised before surgery. The machine which does the sterilisation is called autoclave or steriliser. If sterilisation does not happen or happens insufficiently, life-threatening infections are the result. For this reason the autoclave is one of the most important pieces of equipment in a hospital.
The medical steam autoclave is a device that uses pressurised, high temperature steam to sterilise medical instruments. Although there are still other methods of sterilisation e.g. dry heat, gas (Ethylene Oxide) or gamma radiation, the sterilisation with hot steam is the most common method. The usage is simple, rapid, cost effective and environment friendly. The following article refers to the steam autoclave.
Sterilisation
Sterilisation is the elimination of all transmissible micro organism, bacteria, viruses and fungi from the surface of an instrument. This is different from disinfection, where only organisms are removed by a disinfectant and are not completely eliminated.In general, any instrument that enters the body must be sterilised. This includes all surgical instruments, implants, catheters, syringes, needles, dressings and others.
Proper sterilisation of instruments is crucial in preventing HIV transmission.
Sterilisation is possible with hot air, chemicals or radiation, but the most common method is the use of hot steam, which kills all organisms. This method is easy and cheap to realise.
For a steam sterilisation temperatures above 110°C are needed, which requires the steam to be applied in a pressure chamber. The sterilisation time depends on the temperature. The higher the temperature the faster the instruments get sterile.
Types of autoclaves
All steam autoclaves have a metal chamber to withstand the high pressure and the temperature. A massive door or lid which is locked during operation keeps the chamber closed. The chamber is heated by an electric heating element. In places without electricity supply autoclaves heated up by gas or fuel are common.To ensure that an autoclave works correctly, the machine has a temperature and/or a pressure gauge and often an integrated timer.
Modern autoclaves are all electronically controlled. The control unit controls temperature, pressure and time and monitors all safety functions.
Hospital autoclaves are available with chamber capacities from 5 l to 900 l. The smallest and simplest ones work manually and are heated up by a normal electric or gas stove. The big stationary autoclaves are fully automatically controlled and need three-phase-power supply and a water supply installation.

Pressure cooker type
The simplest autoclave with a capacity of 5-25 l is the pressure cooker type. It is the small and portable version of a vertical autoclave. Usually it is heated by an integrated electric heating element but sometimes it comes without a heater. This version is heated like a pressure cooker on a gas stove. It is made for remote areas without electricity.The pressure cooker type autoclave has a safety valve, a release valve, a pressure gauge and a thermometer. The simplest and cheapest ones come even without a rubber gasket in the lid. The sterilisation process has to be controlled manually by the user. This type is simple, reliable and almost indestructible and very common in small hospitals and small health centres.

Vertical
The vertical autoclave is a stationary top-loader with a capacity of 60 l - 100 l. The construction is simple and robust. The vertical autoclave is often double walled with pressure gauges, thermometer, water level inspection tube and a mechanical timer. Bigger vertical autoclaves need 3-phase electrical installation.Table-top
 Table top autoclaves have a capacity of 20-80 l. Although it has just small capacity, the table-top is the most common autoclave. It is found where
surgical instruments are needed: E.g. in maternity wards, laboratories and at the dentist.
Table top autoclaves have a capacity of 20-80 l. Although it has just small capacity, the table-top is the most common autoclave. It is found where
surgical instruments are needed: E.g. in maternity wards, laboratories and at the dentist. Modern table-top autoclaves are a fully automatically controlled, and often come with a vacuum pump and a drying program for drying the goods after sterilisation.
Table-tops are designed for front loading use and provide different trays for surgical instruments. They also have a safety lock for the door and a water reservoir.
Stationary
 Stationary autoclaves are big, automated or semi-automated machines, built for all sorts of purposes: Instruments, liquids, clothes and even for waste
sterilisation. They are available with capacities up to 800 l. Stationary autoclaves are normally located in the sterile processing department (SPD) of
a hospital. Often the autoclaves have two doors, a front and a rear door and are positioned between two rooms, a sterile and a non-sterile area.
Stationary autoclaves are big, automated or semi-automated machines, built for all sorts of purposes: Instruments, liquids, clothes and even for waste
sterilisation. They are available with capacities up to 800 l. Stationary autoclaves are normally located in the sterile processing department (SPD) of
a hospital. Often the autoclaves have two doors, a front and a rear door and are positioned between two rooms, a sterile and a non-sterile area.Stationary autoclaves require plumbing and 3-phase electrical installation.
The principle of steam sterilisation
The boiling point of water is 100°C (212°F). This means that water cannot be heated above 100°C. Further heating does create steam but does not raise the temperature of the water. Only when water is heated in a closed vessel is it possible to reach higher temperatures. Then the water steam creates a pressure in the vessel. With increasing pressure the boiling point of the water also increases. The temperature gets higher than 100°C and can then be used for sterilisation.Temperature and time
For sterilisation a minimum temperature of 110°C (230°F) is needed. The higher the temperature, the shorter is the needed time to get things sterile. In practice 121°C (250°F) and 134°C (273°C) are defined as the standard sterilisation temperatures for hospital autoclaves.|
Important: Water and steam temperatures of 121°C or 134°C can only be reached under pressure. |
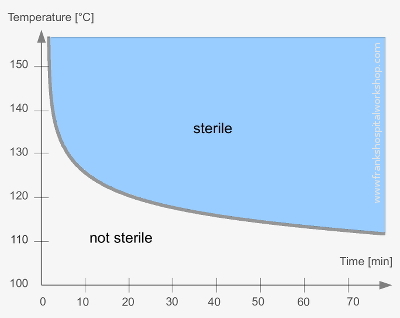

Sterilisation depends on temperature and time. The higher the temperature, the shorter the sterilisation time.
Gauge pressure and absolute pressure
It is confusing. The air pressure at sea level is by definition 1 bar (1013 mbar). This is the true or absolute pressure. The perfect vacuum is according to this definition 0 bar.But our pressure gauges for technical applications always show 0 bar at ambient air pressure. We use a different definition, the so-called technical pressure or gauge pressure. Our zero-point is the normal air pressure at sea level. That means, that 0 bar gauge pressure is equal to 1 bar absolute pressure. That is why we have to be careful and make a clear distinction between absolute pressure and gauge pressure.
Example: 0 bar of a pressure gauge shows us that a vessel is not under pressure. But the absolute pressure is 1 bar. A reading of 2 bar showing on a pressure gauge of an autoclave corresponds to an absolute pressure of 3 bar.
But in practice this fact is not really relevant to us because we are only interested in the gauge pressure or in the change of pressure. We want to know the pressure difference of a pressure-less vessel and a vessel under pressure.
|
Note: We technicians talk about the gauge pressure, the technical pressure. |
Pressure and temperature
In a closed vessel, pressure and temperature rise when the vessel is heated up. When the temperature reaches the boiling point (100°C), steam starts to be generated. This steam creates a pressure. The higher the pressure, the higher the temperature gets in the vessel gets. Pressure and temperature are interdependent. It is not possible that one value increases without the other.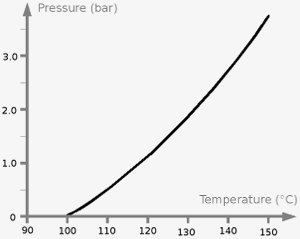
At 121°C the pressure is always 1 bar and if the pressure reaches 2 bar the temperature is always 134°C. Thus, it would be enough to look only at one meter to know if the autoclave works correctly, the pressure gauge or the temperature. But in practice most of the autoclaves have both, a pressure gauge and a thermometer.
Pressure at high altitude
The atmospheric pressure changes with the altitude. At sea level it is 1013 mbar (absolute pressure) but it decreases in higher altitudes. That also means that in higher altitude water reaches the boiling point earlier. It boils at a lower temperature than at 100°C.This also has consequences for an autoclave when the autoclave is pressure controlled and not temperature controlled. When a pressure controlled autoclave at high altitude reaches the 1 bar (gauge pressure) setting and switches off, the temperature has not reached 121°C. The instruments in the steriliser will not get sterile.
For pressure controlled sterilisers we have to increase the pressure limit in order to reach the needed sterilisation temperature. If this is not possible, the sterilisation time has to be longer.
Altitude and pressure
When the autoclave is pressure controlled and the pressure valve cannot be adjusted then it should be done according to the following table.| Altitude | Absolute air pressure | Temperature at 1 bar | Pressure compensation | Temperature at 2 bar | Pressure compensation |
| 0 m | 1.0 bar | 121°C | +0.0 bar | 134°C | +0.0 bar |
| 1,000 m | 0.9 bar | 118°C | +0.2 bar | 132°C | +0.1 bar |
| 2,000 m | 0.8 bar | 117°C | +0.4 bar | 131°C | +0.2 bar |
| 3,000 m | 0.7 bar | 115°C | +0.6 bar | 130°C | +0.3 bar |
| 4,000 m | 0.6 bar | 114°C | +0.7 bar | 129°C | +0.4 bar |
Altitude and time
When the autoclave is pressure controlled and the pressure valve can not be adjusted then the sterilisation time has to be extended according to the following table.| Altitude |
Temperature at 1 bar |
Sterlisation Time |
Temperature at 2 bar |
Sterilisation Time |
| 0 m | 121°C | 20 min | 134°C | 3 min |
| 500 m | 120°C | 25 min | 133°C | 10 min |
| 1,000 m | 119°C | 25 min | 132°C | 10 min |
| 1,500 m | 118°C | 30 min | 132°C | 10 min |
| 2,000 m | 117°C | 35 min | 131°C | 10 min |
| 2,500 m | 116°C | 40 min | 131°C | 10 min |
| 3,000 m | 115°C | 45 min | 130°C | 10 min |
| 3,500 m | 114°C | 50 min | 129°C | 10 min |
| 4,000 m | 114°C | 50 min | 129C | 10 min |
Example 1: In Arusha, Tanzania the altitude is 1,500 m above sea level. A pressure controlled autoclave would reach the 1 bar setting (121°C) already at 117.5°C. If the user would run the normal 121°C-program, the instruments would not be sterile. Either the technician has to adjust the pressure valve to 1.3 bar or if this is not possible, the user has to extent the sterilisation time to 30 min.
Example 2: In La Paz, Bolivia the altitude is 4,000 m. Here we only get a temperature of 114°C when a pressure controlled autoclave switches off the heating element. In order to get the instruments sterile, the '121°C-cycle' has to last 50 minutes instead of 20 minutes or the technician adjusts the pressure valve to 1.7 bar.
Working principle
The working principle of steam autoclaves is always the same. The difference is the control. Manual autoclaves are simple and robust but the user has always to be present. Fully electronic controlled autoclaves are easy to use but more difficult to repair.Working principle of a simple autoclave (pressure type, vertical)
Water is heated up in the chamber. At 100°C steam develops and after a short time the pressure increases, the boiling point of the water rises and so does the temperature (heating phase).When the predefined pressure or temperature is reached the heating element is switched off, either by a thermostat or a pressure switch. In electronic controlled autoclaves a pressure or a temperature sensor delivers a signal to the control board.
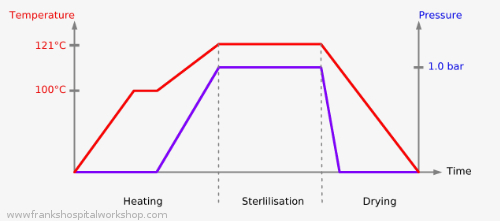
At this point the sterilisation phase begins. Then the temperature drops a bit and the heating element is switched on again. In this way the temperature is kept stable. At the same time a timer gets started and after the set time the autoclave switches off completely. The sterilisation process is now completed (drying phase), the outlet valve opens and releases the steam. The sterilisation goods remain a little longer in the chamber and the radiant heat from the chamber dries the items.
|
Important: The sterilisation time begins only when the sterilisation temperature (121°C or 134°C) is reached. |
Vacuum pump
Unfortunately the sterilisation process is not that easy. In practice the items to be sterilised are not packed separately but in packages wrapped in clothes. When the packages are packed too tight, the steam cannot penetrate everywhere. Zones of colder air come into being and the items do not get sterile.Furthermore some surgical instruments consist of individual parts. In the joints and spaces between the parts little air bubbles with cool air remain and prevent the hot steam to penetrate (e.g. the joints of scissors) and the items will not get sterile.
Simple autoclaves which just use the steam to press the cold air out of the chamber (gravity displacement) have problems to reach the cold air zones in the packs between the instruments. Here an additional vacuum pump helps. Before the sterilisation process begins, the vacuum pump sucks the air out of the packs and the insulating air bubbles disappear (pre-vacuum). Then the sterilisation process is started by the control unit.
Later when the autoclave has finish the sterilisation, the vacuum pump is used again to suck out the steam before the door can be opened (post-vacuum). In this way the packages get perfectly dry.
Working principle of an automated vacuum autoclave
After switching on the steriliser, the vacuum pump sucks the air out of the closed chamber. A vacuum develops, the pressure in the chamber is negative (air removal phase). Then the pump stops, the inlet valve opens and filtered air gets into the chamber as well as distilled water from the reservoir.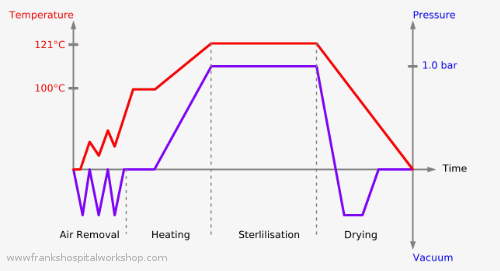
The pressure again is 0 bar. The valve closes and the water heater starts heating. The temperature in the closed chamber rises slowly. In the meantime the vacuum pump creates some more vacuums (air removal phase) which suck the trapped air out of the sterilisation packs. After some minutes the boiling point of the water is reached and the vacuum pump switches off completely. Now steam is created. The steam gets more and creates a pressure. Under pressure the boiling point start to shift and the temperature rises (heating phase). After some more minutes the pre-set temperature or pressure is reached and the heater is switched off.
Now the sterilisation period begins and the timer starts. The pre-set time which is related to the temperature (20 minutes at 121° or 3 minutes at 134°) is counted down. A temperature or pressure sensor controls the whole process and lets the heater restart when the temperature drops (sterilisation phase).
When the sterilisation process is finished an outlet valve opens and steam is released from the chamber, condenses in a special condenser and the hot water gets back into the reservoir. The temperature in the chamber decreases. Now the vacuum pump supports the drying process by sucking the steam out of the chamber (drying phase).
Sometimes a special chamber heater is switched on additionally in order to improve the drying process.
Water quality
The water quality is very important for the usage of autoclaves. In principle only distilled water or de-mineralised water should be used because the water has to be pure and free of any minerals.But often normal tap water is use, which causes serious problems. The tap water leaves deposits on the components of the autoclave and the sterilisation items. Surfaces of surgical instruments get destroyed after some time and valves and the tubing in the autoclave get blocked or damaged. On heating elements a layer of lime is formed which gets thicker and thicker. One day the heating element cannot conduct the heat sufficiently and the heating element will burn out.
 In order to prevent all these problems only distilled water has to be used. The hospital technician should ensure that only distilled water is used and
should check the water quality from time to time. The instrument needed for such a water test is the conductivity meter. It is also sold as aquarium
accessory and is not expensive.
In order to prevent all these problems only distilled water has to be used. The hospital technician should ensure that only distilled water is used and
should check the water quality from time to time. The instrument needed for such a water test is the conductivity meter. It is also sold as aquarium
accessory and is not expensive.When distilled water is not available, sometimes drinking water is an alternative when it does not contain minerals. In some places drinking water is processed by reverse osmosis plants. In this case you can also take this drinking water. But also here, you should test the water first with a conductivity meter.
Another alternative is filtered rain water. Rain water is in principle free of minerals and thus perfect for an autoclave.
Using the autoclave
The user has to be trained in the correct usage of the autoclave. They have to know how to run the different sterilisation programs and how to clean the autoclave after usage. This instruction in the operation of an autoclave should be given by the hospital technician with the help of the user manual.But beside the correct usage of the machine the preparation of the sterilisation goods is even more important. The cleaning and packing has to follow strict international guidelines and has to be carried out by qualified personnel only. To perform such a user training is however not the task of the hospital technician.
Precautions for usage and service
Be very careful while operating and servicing an autoclave. Autoclaves generate extreme heat and high pressure. Simple autoclaves only have little or no heat shielding around the chamber.Do not place paper, cardboard, plastic or flammable liquids next to an autoclave.
The operation has to follow exactly the user manual of the manufacturer.
In addition, always consider the following safety precautions:
1. Make sure that the chamber is filled up with enough water.
2. Check if the door gasket is in place and the door is locked firmly before starting the
autoclave.
3. After sterilisation make sure the autoclave is switched off.
4. Make sure that the chamber is pressure-less and cooled down before opening the door.
5. Open the door slowly, keeping head, face, and hands away from the opening.
6. Wait at least 30 seconds after opening the door before reaching or looking into the
autoclave.
7. Remove solutions from the autoclave slowly and gently. Some solutions can boil over
when moved.
8. Clean up any spills immediately.
9. Hospital staff should report any malfunctions or accidents immediately.
User manual
The usage of the autoclave has to be followed strictly according the user manual. One copy of the user manual has to present in the department where the autoclave is operating and one should be available in the workshop.It is also a good idea to create a 'Quick User Chart', a one-page to-do-table with the most important information for the operator. Additionally, the phone number of the hospital technician should not be missing. This instruction can be laminated in plastic and hang up close to the autoclave.
Using a vertical autoclave
The following is an example for the usage of a standard vertical autoclave. Every single step has influence on the quality of the sterilisation. Any mistake results in unsterile or wet packages.1. Fill the autoclave with the right amount of distilled water.
2. Place a Bowie-Dick indicator strip in the centre of the load. (see ↓Bowie-Dick-test)
3. Load the autoclave with the packs. Do not overload. Packs must not touch the chamber
wall.
4. Close the lid tightly.
5. Open the air outlet valve so that the air can escape when heating up the autoclave.
6. Heat up the autoclave.
7. After water is boiling and all cold air is escaped, close the air outlet valve.
8. After some minutes when the pressure reached 1 bar (15 psi) reduce the heat and start
the timer. The sterilisation time is shown in table ↑Temperature and time.
9. When sterilisation time is over, turn off the autoclave or the gas supply and let the
autoclave cool down. At 80°C the vent valve can be opened and after this the lid. This
step may differ from one manufacturer to another.
10. It is a good idea to keep the packs in the warm autoclave for a while so that the
packs can better dry.
Cleaning by the user
An autoclave has to be perfectly clean at all times. It is the operators who are responsible for the condition of the autoclaves. Together with the hospital technician they should think about an appropriate procedure and schedule. This plan should be adapted to the situation on site. If the water quality is not perfect and the cleaning technique of the user also not sufficient, then the autoclave has to be cleaned more often.A typical procedure for cleaning is the following:
Daily (by the user)
1. Remove and clean the outlet sieve under running water.
2. Clean the chamber using a cloth. Do not use abrasive cleansers or steel wool, as these
will scratch the surface and increase corrosion.
3. Clean the trays or baskets with multi-purpose cleaner and a cloth.
4. Clean the door or lid gaskets with a cloth and check for defects.
5. Do a performance test by using indicator strips (see ↓Bowie-Dick-test).
Weekly (by the user)
1. Flush the chamber drain to keep it free of residues.
2. Remove the outlet sieve. Pour 1 litre of multi-purpose cleaner and hot water down the
drain with a funnel. Rinse drain with 1 litre of hot water. Clean the sieve with multi-
purpose cleaner and put it back into place.
3. Do a performance test by using indicator strips.
Bowie-Dick-test
We technicians check the temperature and the sterilisation time to ensure that the autoclave meets the technical conditions for the sterilisation process.A performance test does more, it shows if the whole sterilisation process was successful, if the packages were packed correctly and the autoclave not overfilled.
Such a test is performed with indicator strips or tape and is called Bowie-Dick-test.
According to the international standards Bowie-Dick-test has to be done every day by the autoclave operator.
For this purpose a test strip is placed in the centre of the load and the sterilisation cycle is started. After sterilisation a colour change indicates whether the steriliser works correctly or not. A failed test can be the result of a defect autoclave or, and this is more likely, of an overfilled or wrongly packed autoclave.
When a Bowie-Dick-test fails and the operator does not find a packing problem, the hospital technician has to come to do a technical check. Then the sterilisation temperature and the time have to be measured.
To do a Bowie-Dick-test in the workshop after maintenance or repair is pointless because we run the autoclave empty and a Bowie-Dick-test would always pass.
In addition to the daily Bowie-Dick-test, a more precise test with biological indicators should be done twice a year. These indicators have to be sent for analysing to a certified laboratory.
Validation
An autoclave validation goes even further. A validation monitors the whole sterilisation process from the cleaning and packing to the sterilisation process and unpacking. It also covers technical issues like measuring the sterilisation temperature but mainly the organisational aspects.For validation national or international standards apply.
Common problems during usage
During the sterilisation process some problems can occur. Here are the most common ones:Wet material after sterilisation
This is probably not a technical problem. It is more likely that the autoclave is overloaded, the air-release valve was not opened completely, the door was not briefly opened after sterilisation, or the packs are too close to the wall, etc. However, the only correct way to achieve the best drying result is described in the user manual and the operator should follow these instructions.
Basically, the wet steam has to be released out of the chamber after the sterilisation. If this does not happen the steam will condense, becomes water and the sterilisation goods become wet. A typical procedure to improve the drying is that the user opens the door briefly after sterilisation so that the steam can escape and then leave the door ajar.
But this is only one possibility. There is no general perfect method. Every autoclave is different. So please read the user manual!
Door locked after power outage
After a power failure many electronically controlled autoclaves are reset and are not able to continue the sterilisation cycle. The chamber is under pressure, contains hot steam and hot water and the door is locked by the safety lock mechanism. The user manual explains how to open the door in this case. But be careful, hot steam and hot water will escape when opening the door.
Here are some more suggestions to prevent problems during usage:
 Use only distilled water. Never use tap water.
Use only distilled water. Never use tap water. Use towels to separate instruments and absorb moisture if needed.
Use towels to separate instruments and absorb moisture if needed.  Hinged instruments must be autoclaved in the open position.
Hinged instruments must be autoclaved in the open position. No sharp instruments should be allowed to touch other instruments.
No sharp instruments should be allowed to touch other instruments.  Do not over-pack the autoclave. Otherwise, steam does not get everywhere.
Do not over-pack the autoclave. Otherwise, steam does not get everywhere. Make a daily performance test.
Make a daily performance test.Steam-pulsing
Pressure cooker types and vertical autoclaves without a vacuum pump have problems to remove the air of porous sterilisation goods. In this case some experts suggest to use the steam-pulsing technique in order to improve the sterilisation result.Therefore, the air-removal valve is opened and closed briefly for a few times at the beginning of the sterilisation phase. These pressure pulses flushes out the trapped air in the porous sterilisation goods. The sterilisation phase has of course to be extended by a few minutes.
This method really works fine for sterilisation of porous sterilisation goods. But to make it clear: It is an improvement for an otherwise functioning procedure.
The steam-pulsing method is no solution for wrong usage and it cannot replace the procedure described in the user manual. Instead of implementing another (complicated) procedure, make sure that the operator first follows the instructions in the user manual.
Construction of a vertical autoclave
The typical vertical autoclave is manually controlled and very common in smaller hospitals. The components are simple and can be repaired and replaced easily.Such an autoclave consists of the following parts:
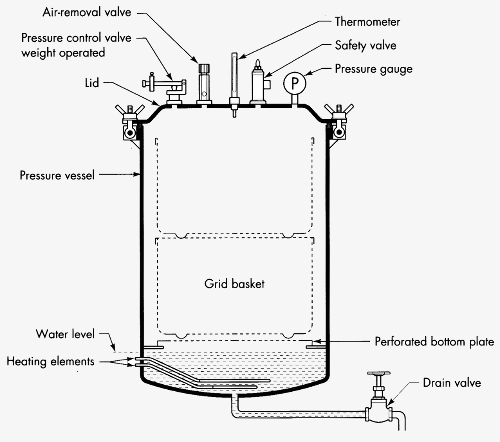
Pressure control valve
The pressure control valve opens when the working pressure (and thus the temperature) is reached. It works with a counter weight or a spring and can be adjusted manually.Air-removal valve
Is opened manually when the sterilisation process is finished. It releases the steam out of the chamber. This can be done by opening a mechanical valve or by a solenoid when pushing a switch.Thermometer or temperature gauge
The thermometer shows the temperature inside the chamber and thus indicates to the user when the sterilisation temperature is reached and the sterilisation process can be started.Safety valve
The safety valve opens and releases the pressure out of the vessel if the pressure control valve fails and the pressure gets too high.With pulling the safety valve also the steam pulse can be applied (↑Steam-pulsing)
Pressure gauge
The pressure gauge shows the pressure in the vessel but is not really needed when a thermometer is built in.Lid and lid gasket
A heavy lid closes the vessel airtight. The lid is sealed with a silicon gasket. The gasket has to be checked and cleaned frequently. A leaking gasket allows hot steam to escape and can create serious burns.Pressure vessel
The high pressure chamber is made out of stainless steel. It contains the sterilisation goods.Heating element
The heating element (sometimes three elements for a three-phases power supply) heats up the water. It is important that it is always covered with water. A dry heating element will burn out within seconds.Drain valve
It is used to drain remaining water from the chamber after sterilisation and during cleaning.Variations
Some vertical autoclaves are double walled where the sterilisation goods are not placed directly over the heated water in the upstream steam but in another chamber. This inner chamber is placed in such a way, that the steam can only enter from above. That helps to achieve a more homogeneous and safer sterilisation result.Because the water level is no more visible in a double walled autoclave, this type has a gauge glass that shows the water level inside the outer chamber.
Most of the autoclaves have an integrated timer. The timer starts when the sterilisation temperature is reached and switches off the heating elements when the sterilisation time is over. The timer is often a mechanical one, driven by a little motor. In modern autoclaves the timer is a small electronic circuit.
Circuit diagram of a semi-automated vertical autoclave
Here a circuit diagram of a typical vertical autoclave with some interesting features such as a timer and a low-water protection.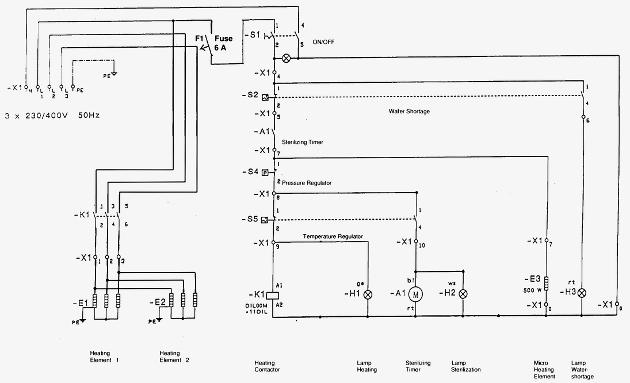
The circuit diagram consists of two parts: On the left the three-phase power circuit with the heating elements and on the right side the single phase control circuit.
At the top left we find the mains power supply input. The contactor K1 is connected to the mains power supply and switches the two triple heating elements (in parallel) on and off.
The coil of the contactor K1 we find in the right part of the diagram. This part runs on single phase (via the main switch, fuse F1 to L1). The common reference point is N (neutral) which also comes from the mains.
The solenoid is activated when the thermostat S5 is not closed, the pressure sensor S4 below the release point, the timer A1 is wound up, the water level is sufficient (S2) and the autoclave is switched on by S1.
When winding up the timer, the switch A1 closes, the heater can be started but the timer itself does not run because the timer part of S5 is open. The switch will only close when the sterilisation temperature is reached. Then the other part of the switch opens the contactor part.
Tricky also the low-water detector. This detector consists of two parts, the micro heating element E3 and the temperature sensor S2. This sensor has nothing to do with the sterilisation temperature. In fact the release temperature is clearly higher than the sterilisation temperature. This thermostat is mounted directly to the micro heating element next to the main heating elements in the water. If everything is OK, the thermostat does not get hotter than the sterilisation temperature. But if the water level is too low, the micro heating element cannot emit the heat to the water, gets much hotter and the thermostat switches off the whole system.
Construction of a table top autoclave
The general function sequence of a table top autoclave is the same as for a manual vertical autoclave. The only difference is, that a table top autoclave runs semi- or fully automatically.After the door has been closed, the autoclave can be started.
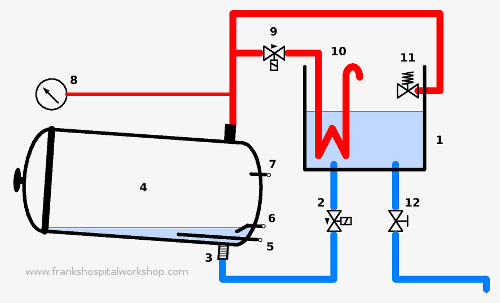
The valve 2 opens and water runs from the reservoir 1 through a filter 3 into the chamber 4. When the water level reaches the level sensor 6 the valve closes and the heater switches on. After a while, steam is generated. The steam rises and pushes the cooler air through valve 9 and the condenser 10 out of the chamber. When the temperature reaches the boiling point (measured by the temperature sensor 7), the outlet valve 9 closes. Then the pressure in the chamber rises (shown by the pressure gauge 8) as well as the temperature. When the sterilisation temperature is reached (sensor 7), the heating element switches off. If the temperature control fails and the pressure gets too high, the pressure is released by safety valve 11. For cleaning and servicing, the water can be drained by the manual valve 12.
In addition, modern table top autoclaves provide more safety features like a door lock and an internal water tester and most of all a suction pump. Mechanical sensors and meters are replaced by electronic ones. An electronic board or a microprocessor controls and monitors the sterilisation process.

1 Heating element
2 Water inlet
3 Level sensor
4 Steam to reservoir
5 Test port for external
thermometer
6 Safety valve
7 Sensor for thermometer
8 Pressure meter
9 Sensor for temperature
control
Door lock / door switch
Only after closing and locking the door properly can the steriliser be switched on. A micro switch at the door mechanism gives the information to the electronic board and a solenoid blocks or releases the door mechanism.Level switch for water inlet
A certain amount of distilled water is let into the chamber automatically. The water intake is either time or level controlled. In the second case a water sensor in the chamber is needed. It is usually just a piece of metal that works as a sensor together with a little electronic circuit. This circuit measures the electrical resistance between the sensor and the chamber. When water reaches the sensor the resistance becomes low and the electronics switches off the inlet valve or the water pump.Temperature sensor
The actual temperature in the chamber is measured by a temperature sensor. The sensor delivers the measurement to the control unit. Here the actual and the pre-set temperature are compared and a control voltage for switching the heating elements is created.Chamber heating / thermal fuse
Often the outside of the chamber is also heated. This heating supports the drying process after sterilisation.This chamber heating is usually protected against over-heating by a thermal fuse.
Steam valve
After the sterilisation phase, the release valve (outlet valve) opens. Steam gets out of the chamber, flows through a condenser and gets back as hot water into the reservoir.Safety valve
The safety valve is designed to release steam in case the chamber pressure is increasing beyond the normal range due to a fault in the control elements. Without safety valve the chamber would burst with catastrophic consequences.Variations
Modern table top autoclaves always provide a vacuum pump. Whenever a vacuum pump is used, an additional ventilation valve with a bacterial filter is needed.Often table top autoclaves also have an internal water quality tester. Before the distilled water is led into the chamber, the water conductivity is automatically tested. When the quality is not good enough, the autoclave cannot be started.
Construction of a stationary autoclave
Large stationary autoclaves, especially when they consist of several sterilisation chambers are run by steam from an external water boiler. The advantage is that hot steam is available immediately, the pressure in the chamber builds up faster and the overall sterilisation time gets shorter. When the sterilisation of one batch is finished, the next batch can already be loaded and started.Additionally, each chamber is surrounded by an outer shell, the jacket. Here hot steam circulates and pre-heats the chamber before it is used.
Also the chamber is post-heated that way when the steam is released out of the chamber after sterilisation. This prevents water condensation and ensures a dry sterilisation result.
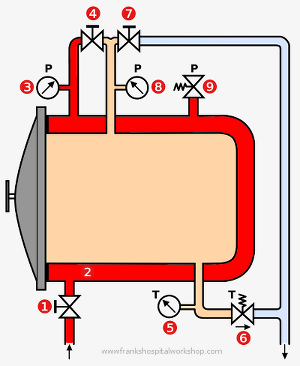
When the inlet valve 1 is open, hot steam from the external boiler enters the jacket 2 of the autoclave. The chamber gets preheated. The pressure gauge shows 3 the jacket pressure. When valve 4 is opened, the steam gets into the chamber. The colder air escapes through the open valve 6. The valve is a temperature controlled one-way valve. The valve closes when the steam is hot enough. Now the pressure rises until it is as high as the inlet pressure. The chamber pressure is shown by the pressure gauge 8 and the temperature by the thermometer 5. It is placed at the bottom of the chamber, where the lowest temperature is. When the sterilisation time is over, the inlet valve has to be closed and the outlet valve 7 opened. Steam escapes through the drainage pipe. The pressure and the temperature in the chamber decrease but the jacket is still under hot steam pressure. This supports drying the load. After a while the steam from the jacket can also be released by opening valve 4 or it can be kept if another load has to be sterilised.
The safety valve 9 opens when the steam pressure is too high. In principle this valve is not needed because the boiler already contains one and the pressure in jacket and chamber cannot get higher than the pressure in the boiler.
Variations
Simple, manually controlled autoclaves are still widespread. They are robust and relatively easy to repair. Spare parts can be found in every larger city. Modern stationary autoclaves are fully electronically controlled. There are no more manual valves and also the instruments for pressure and temperature are often digital ones.Also in stationary autoclaves a vacuum pump provides a better sterilisation result and has already become standard. Wherever a vacuum pump is used, an additional ventilation valve with a bacterial filter is needed to ensure only uncontaminated air can enter the chamber when equalizing the pressure at the end of the cycle.
Maintenance
Beside the routine checks by the user personnel, autoclaves should be maintained at least once a year by the technicians of the hospital workshop. Many manufactures suggest even semi-annual maintenance according to their guidelines.The maintenance of an autoclave covers the cleaning from inside and outside, a functional check and the control of the temperature. A calibration has to be done if the temperature check was not successful.
Very often a service manual is needed to set the autoclave in a defined service mode and to find the calibration points for the temperature and the display.
|
Note: Be very careful while doing service on an autoclave. Some older autoclaves have
only little or no heat shielding around the chamber. The chamber, tubes and valves get very hot. |
Needed tools
Beside the standard tools you need a calibrated thermometer with an external sensor. Only with such a reference thermometer are you allowed to check and adjust the temperature. The built-in (digital) thermometer of the autoclave cannot be taken for the temperature check. When the display of the autoclave does not show the correct temperature you do not really know if the temperature is wrong or the thermometer itself shows a wrong result.For some models it is useful to have a 2 mm rod sensor which can be inserted in a special test port.
More under ↓Calibration.
A pressure meter is not needed, even if the manufacturer recommends this. Stay with the temperature measurement. It is safer, more practical and cheaper.
The maintenance should also include a water conductivity test. A lot of problems with autoclaves are caused by the usage of water of poor quality.
More under ↑Distilled water.
Then, we need of course cleaning material like: A bucket, dish washing liquid, a sponge and a stainless steel scouring pad.
Maintenance procedure
A typical annual or better semi-annual maintenance procedure is the following:1. Fill steriliser with distilled water.
2. Place temperature sensor for external thermometer in the centre of the chamber.
3. Perform a test run at 121°C.
4. Check the temperatures inside the chamber. If it is lower than 121°C, do a calibration.
↓Temperature calibration
5. Check the display of the internal thermometer. Adjust it if necessary.
↓Temperature calibration
6. Check the function of the safety valve. Pull a few times with long pliers or a
screwdriver when the chamber is under pressure. Be careful, hot steam will come out.
7. Monitor the sterilisation time with a stop watch, your watch or your mobile phone.
8. Do a visual check for leakages from inside and outside.
Let the autoclave cool down and then continue:
9. Clean chamber, heating element and rinse the drainage (see ↓Cleaning).
10. Clean or exchange the drainage filter and the air filter.
11. Check door gasket for damages. Lubricate gaskets with silicon oil.
12. Lubricate door hinges and check the door closing mechanism.
13. Visual check for leakages: chamber, door, piping, valves, water reservoir.
14. Check electrical connections.
15. Check the electronic board for cold solder points and water damages.
16. Check contacts of relays.
17. Make a final test run at 134°C.
18. Do a calibration for the temperature display if needed.
19. Replace cover.
20. Drain the water and clean the autoclave from outside with soap water.
21. Fill out the maintenance protocol.
Cleaning by the technician
It is the task of the user to keep the chamber clean, as well as the autoclave from outside. The user has to clean all parts which are visible and reachable on a weekly or monthly base. The technician however must be able to demonstrate the correct cleaning to the user.Everything that needs disassembling for cleaning is the task of the technician, which includes cleaning of filters, valves and pipes and the heating element.
The correct cleaning of an autoclave is very important not only to achieve a satisfactory sterilisation result but also because most of the technical problems are created by residues due to insufficient cleaning after sterilisation.
It is advisable that the technician starts with general cleaning as described above under ↓Cleaning by the user.
Then, we can continue with our 'technical' cleaning:
1. Drain the water from the reservoir. Clean the reservoir with a sponge and distilled
water or with a soap solution if needed.
2. Remove the water filter (between reservoir and chamber). Rinse it under running water
in reverse direction.
3. Remove also the water outlet filter which is found at the bottom of the chamber. Rinse
this filter under running water.
4. The air inlet filter for ventilating the chamber after sterilisation has to be replaced once
a year.
5. Do not forget to rinse all the cleaned parts with distilled water when you are finished.
6. If the hospital uses rain water, make sure that the water is filtered before it gets used
for the autoclave. In case of a doubt, talk
with the operator and find a solution. Maybe an additional filter (e.g. a fuel filter from
a car accessory shop) can be added.

Limestone
Often the chamber and the heating element are covered with lime scale and the tubes and valves are blocked with lime deposits.The chamber can be cleaned by scraping of the scale with a scouring pad which is used in the kitchen for cleaning pots and pans. Avoid steel wool, as steel wool scratches the metal surface of the chamber.
Heating elements should be handled with care. They are made from soft copper or brass pipes and are then coated or chrome-plated. They are less durable than the thick stainless steel of the chamber. If you want to remove lime scale from a heating element by scratching, you will destroy the surface of heating element. The copper tube of the element is then visible and it will not take much time until holes appear. That is very dangerous because the intruding water creates an electrical connection to the power supply. The whole autoclave is then under power then, which is particularly dangerous when the electrical installation is poorly done and no earth-leakage circuit breaker is installed in the mails supply.
The best way to remove limestone from a heating element is to remove the heating element and put it in de-scaler which is used for water kettles and coffee machines and leave it over night. Vinegar also works, but it takes longer. You can also try denture cleaner.
| Do not forget, better than removing limestone is to prevent it. Teach the operators in the correct cleaning and ensure that they are using distilled water only. |
Temperature calibration
For the calibration you need an external calibrated (digital) thermometer. Only with such a reference meter are you allowed to calibrate the autoclave. Never trust the internal thermometer.The calibration of the equipment is only as good as your measurement device. Do not use the cheapest and keep in mind that even the expensive ones have to be calibrated after some time.



Inexpensive quality multimeter with thermometer adapter.

High quality multimeter with 2 mm sensor. This sensor fits e.g. into the test port of Eschmann table top autoclaves.
In principle the calibration of an autoclave consists of two adjustments. First the calibration of the control unit and then the adjustment of the internal thermometer. Again, never do the calibration according the internal instrument.
Insert the sensor of your reference thermometer into the chamber and close the door. The rubber gasket prevents the cable from being damaged. Start the autoclave. The gasket might not be perfectly sealed now and some steam will escape. Technically it does not matter as long as more steam is created than can escape and the pressure rises. But do not burn yourself.
The calibration procedure varies from case to case. Do the calibration always according the service manual of the manufacturer. If no manual is available, you have to do the calibration by yourself. In a simple case you find two trimmer pots on the control board. One trimmer pot is for 121°C and the other one for 134°C. Start with the temperature calibration.
 Memorise the original settings of the trimmers. Or better make a sketch or mark them
Memorise the original settings of the trimmers. Or better make a sketch or mark them with a pen. For adjusting a ten-turn-trimmer count the turns.
 Make changes only in small steps.
Make changes only in small steps. Keep in mind that changes of the temperature setting need some time to take effect. Turn
Keep in mind that changes of the temperature setting need some time to take effect. Turn the trimmer only a little and wait until the temperature is stabilised.
 Cheap trimmers are not insulated. Be careful by inserting the screw driver that you do not
Cheap trimmers are not insulated. Be careful by inserting the screw driver that you do not make a short to other metal pieces.
After the temperature is set, the thermometer can be adjusted if necessary.
There should be also a trim-pot for the thermometer close to the display where it can be calibrated. Mechanical meters can be adjusted by turning a little screw which shifts the pointer. With round meters the scale often can be twisted or even the whole meter housing. If all this does not work, keep in mind it is just a meter. It has nothing to do with the function of the equipment. Also a calibrated autoclave with an inaccurate thermometer performs a safe sterilisation. But then you have to inform the user.
Installation
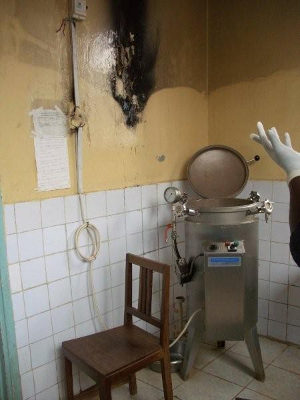 When a new autoclave has to be installed, some preparations have to be done beforehand. We have to prepare the electrical installation, the water
supply and the water drainage. Sometimes also a tap water connection is needed when the autoclave has an active cooling system. Or an additional
water distiller has to be installed.
When a new autoclave has to be installed, some preparations have to be done beforehand. We have to prepare the electrical installation, the water
supply and the water drainage. Sometimes also a tap water connection is needed when the autoclave has an active cooling system. Or an additional
water distiller has to be installed. The electrical installation needs a circuit breaker for each phase and should have a 30 mA earth-leakage circuit breaker. Note the power consumption and choose the right fuses and wire size.
For a 230 V system up to 3.5 kW a 16 A circuit breaker is fine and a 1.5 mm² cable can be used. For higher currents up to 21 A, a 2.5 mm² cable has to be used.

Here an undersized main switch caused a fire
The autoclave also has to stand perfectly horizontal. If not, the water amount which is let in the chamber and detected by a level sensor can be wrong.
Repair
Before starting a repair... read the user and the service manual of your autoclave.
read the user and the service manual of your autoclave. fill out a service record/job card with all equipment data and the fault description.
fill out a service record/job card with all equipment data and the fault description. make sure that distilled water is available in your workshop when you repair a table-top
make sure that distilled water is available in your workshop when you repair a table-top in your workshop.
Error code
In case of a fault, microprocessor controlled autoclaves show an error code in the display. With the help of the service manual the fault can be identified easily.Typical technical problems
Below some typical problems in connection with autoclaves:Burnt-out heating elements
Burnt-out heating elements are the number one problem with autoclaves in hospitals with poor maintenance service.Pressure cooker types or vertical autoclaves are often used with too little or without water. Then the heating elements burn out within seconds.
Or the heating elements are covered with lime scale. Then the heating elements cannot give off the heat, get overheated and will also burn out. (Removing lime scale see ↑Lime scale.)
It is also possible that the water supply is blocked with debris or the water level sensor delivers a wrong signal. This happens when the water sensor is dirty. Then the control unit measures a resistance and 'thinks' that there is already enough water in the chamber and switches on the heating elements.
Therefore it is important not only to change a burnt heating element but also to look for the reason. Make sure that the chamber really is filling up with water. When you start a table top autoclave, look into the water reservoir and check if the water level in the tank falls.
Heating elements are not repairable. We have to get a replacement either from the manufacturer directly or try to find a similar one somewhere else. Universal heating elements might be available in the repair shops in bigger town. These are spare parts for water heaters which can also be used for autoclaves. But it is not so easy to find the right one. The mounting and the shape of the heating element must be similar because it has to be covered with water all the time. It is no problem if the wattage is slightly smaller or bigger. The sterilisation will then take just more or less time.
It is advisable to have a spare heating element in stock and if you have more than one autoclave of the same type in your hospital, it is a must.

Solid state relays
The heating elements are switched on and off by electromechanical contactors or in modern autoclaves by solid state relays. These relays do not contain mechanical contacts but a so-called triac.The function of the mechanical relays is clearly to see and to hear but there is nothing to see and hear of a solid state relay. Even the voltage measurement can be confusing, because the frequency of switching can be much faster. While mechanical relays are switched on and off every 10 to 30 seconds, the solid state relays can be triggered in milliseconds. This switching is faster than our voltmeter and as a result we measure an average voltage. This 'reduced voltage' is correct and not an unwanted voltage drop.
Leaking door gasket
Rubber gaskets get hard over time and crack. A leaking gasket will not necessarily affect the performance of the autoclave. As long as the heating element produces more steam than escapes trough the leakage, the autoclave will work. But the escaping steam is of course dangerous for the user and thus the gasket must be exchanged.The gaskets should be checked and cleaned weekly and lubricated with silicon oil during the maintenance.
After removing a silicon gasket it is sometimes difficult to put it back into the groove of the lid or door. It seems to be too long. Do not inserting the gasket bit by bit around the lid but start with inserting it at the 12 o'clock position, then continue at 6, 3 and then 9 o'clock.
|
TIP! DIY Door Gasket The door gasket usually lays in a groove. If the gasket is damaged and no exchange part is available, it is possible to make a gasket by filling out the groove with elastic silicone. Once dried the silicon is elastic, durable and heat resistant. Silicon cartridges are cheap and available in hardware stores. Take off the door and lay it flat on the workbench. Check the thickness of the old gasket and take it out. Clean the groove thoroughly with soap water and then with alcohol. Get a small flat bowl with dishwashing liquid and some rugs or paper tissues. Prepare the silicon cartridge and the pump. Fill the groove with the silicon. Now flatten the silicon with a finger. To do this, wet the finger with dishwashing liquid glide over the silicon so that it gets flat and even. Keep your finger always wet or the silicon will stick to your finger and the silicon surface gets destroyed. After finishing, the silicon has to dry. This can take a few days depending on the thickness. After drying, mount the door and check if the door closes properly. Make a test run and check for leakages. |
Water level sensor
Often the water level in the chamber is detected by a piece of metal and a conductivity measurement circuit. When the sensor gets wet the resistance against the metal chamber gets low and the connected electronics switches the water inlet valve off and the electrical heater on. But this also happens when debris bypasses the sensor. In this case the heater starts without water and a damaged heating element is the consequence.

Here the level sensor touches the heating element. As the result of this short circuit to ground the control 'thought' that already enough water was in the chamber. The water inlet was kept closed and the heating element was started. Some of the sterilisation goods caught fire.
The sensor has to be clean and free of debris. Check also the insulation and the mounting of the sensor. But it is better to remove the sensor and clean the individual parts.
The autoclave also has to stand perfectly horizontal. If not, the amount of water which is let into the chamber and detected by the sensor can be wrong.

Thermostat and mechanical Thermometer
Mechanical thermostats and thermometers are common in simple autoclaves. Both consist of a sensor and a pressure can. The sensor is a thin capillary tube which leads into the pressure can (or expansion chamber). This chamber has a moveable metal lid or diaphragm. This closed system contains a liquid or gas which expands when getting warmer. The lid moves and activates a connected electrical switch or in case of a thermometer moves the pointer of a meter.The thin capillary tube is often rolled up. This is correct. Do not cut it. It is not a wire. Also avoid bending the tube. It can get kinks and will then not work any more.

Temperature switch or fuse
When the autoclave is heated up by a chamber heater (a heater around the chamber), the chamber heater is connected to a temperature switch or fuse. This switch is mounted at the outside of the chamber and protects the chamber heater from over-heating in case the electronic control fails.In case this fuse is burned or the switch is triggered there must be a reason and you should find out.

Safety valve
Check the safety valve for correct operation when the autoclave is in operation. Do not burn yourself. Take pliers to pull the metal pin to release some steam. Be careful - do not burn yourself!Pull several times. This cleans the mechanism from possible debris, which can easily block the release mechanism.
Black or burned relay contacts
Black relay contacts can be perfectly cleaned with a fibreglass brush. Never file contacts. This destroys the surface of the contacts.Wet material after sterilisation
This is unlikely to be a technical problem. See ↑Common problems during usage.After the repair
 When the autoclave is repaired, continue with a full maintenance procedure as described
When the autoclave is repaired, continue with a full maintenance procedure as described under ↑Maintenance including a thorough cleaning.
 Make a test run with a temperature check.
Make a test run with a temperature check. Finally, fill out your job card/service report and put a new service sticker to the autoclave
Finally, fill out your job card/service report and put a new service sticker to the autoclave showing the next maintenance date.
 Before returning it to the laboratory, make sure the autoclave is complete with all trays
Before returning it to the laboratory, make sure the autoclave is complete with all trays and baskets.
Service manual
Service manuals are hard to come by. Some manufacturers are helpful and send a copy on request, but most of the manufacturers do not.If you need a manual you can also check here.
Spare parts
It is advisable to have a spare heating element in stock and if you have more than one autoclave of the same type in your hospital, it is a must.The same applies to door gasket. It is only a matter of time when a door gasket will leak. Put one in stock.
Filters should also be kept in stock, especially bacterial filters which are disposable and cannot be cleaned.
Alternatives for steam sterilisation
Some products such as plastics, paper and liquids cannot be exposed to high temperatures or humid air and sterilisation has to be done in different way.Alternatives are dry heat provided by hot air ovens or sterilisation using specific gas through gas sterilisers.
Hot air ovens
Dry heat can also be used to sterilise products but is less efficient than the sterilisation with steam. The process takes longer and the temperature has to be higher. Dry heat is used for the sterilisation of some plastics, papers, special liquids and powders which cannot be sterilised with steam.One advantage of dry heat is, that it does not cause rusting of steel products.
The hot air can be applied without high pressure.
The standard setting for a hot air oven is:
 160°C (320°F) for 120 minutes
160°C (320°F) for 120 minutes 190°C (374°F) for 12 minutes
190°C (374°F) for 12 minutes|
Note: Hot steam at 134 °C can achieve in 3 minutes the same sterility as hot air at
160°C in two hours. |
Gas steriliser
Some specific types of gas can also be used for sterilisation. Ethylene oxide is such a gas which is used in special gas steriliser. It is a chemical agent that kills micro-organisms, including spores.Because a mixture of ethylene oxide in air is explosive and toxic, the gas technology is complex and expensive and is only used where steam sterilisation cannot be used.
The sterilisation process with gas depends on the gas concentration, temperature and humidity but generally it takes much longer than the sterilisation by steam. A typical sterilisation by ethylene oxide takes 16-28 hours at 50-60°C. After sterilisation, all materials have to be ventilated at least 24 hours before contact with the skin.
Links and sources
Here are some Wikipedia Medical Equipment articles:Autoclave
Autoclave tape
Sterilisation
Pressure
Pressure measurement
 You can read the revised article in the book:
You can read the revised article in the book: Introduction to Medical Equipment Repair The book also contains a chapter on preventive maintenance, with recommendations on how to perform the various tests. Click here for more information. |
 |
 |